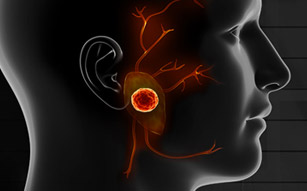
FOLLOWING THE REMOVAL OF THE PAROTID GLAND due to tumor, enlargement, or inflammation, a portion of the face is left hollow where the gland used to be. During parotid reconstruction surgery, our team of specialists at the CENTER will meticulously correct the defect to restore harmony to the face and prevent long-term complications.
WHY IS PAROTID RECONSTRUCTION NECESSARY?
When the parotid gland is removed during a parotidectomy, and a reconstructive procedure is not immediately performed, patients commonly experience a dramatic change in their appearance. In many cases, they are left with a hollow divot that results in an asymmetrical appearance, as well as sagging skin from the removal of an excessively large parotid gland and tumor.
Additionally, failure to reconstruct the area means that the delicate facial nerve is now exposed, covered only by a thin layer of skin. This can lead to the development of Frey’s Syndrome – a condition in which the facial nerve branches that aid in saliva production inside the parotid gland start to grow into the skin and attach to the sweat glands. This causes excessive sweating on the side of the face when the patient is hungry or eating. Performing parotid reconstruction at the time of the parotidectomy prevents the patient from developing Frey’s Syndrome.
PAROTID & PLASTIC SURGERY
LARGE PAROTID TUMOR RECONSTRUCTION
FACIAL DEFECT
Once the parotid is removed, if the skin is placed down on the remaining residual parotid tissue, it will stick to the gland. This will create a
hollowness proportionate to the amount of parotid gland removed. This asymmetry is quite visible as a divot on the side of the face & neck.
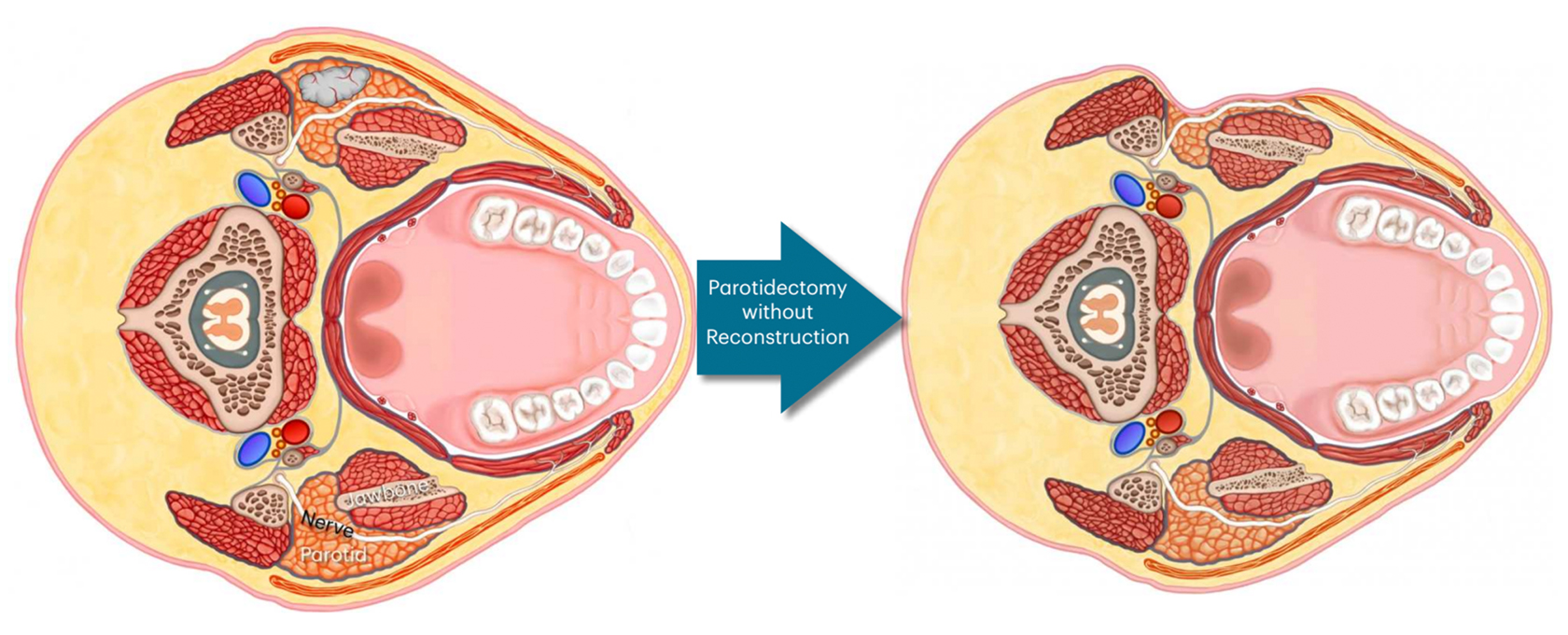
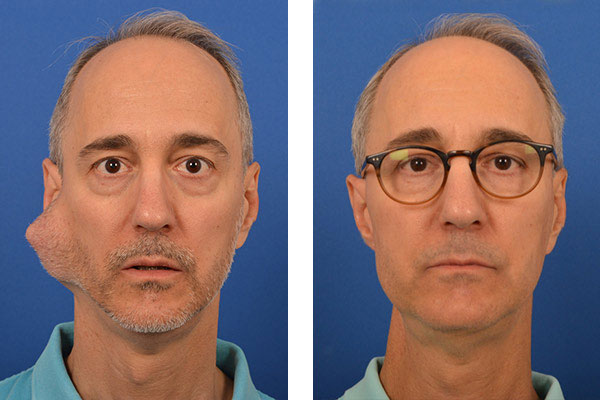
Often, we at the CENTER have to repair and reconstruct the defects from parotidectomies performed elsewhere. In most places, parotidectomies are done through the full incision (Modified Blair Incision that extends into the neck) and without reconstruction (as in the patient below). This can be very challenging but also very fulfilling.
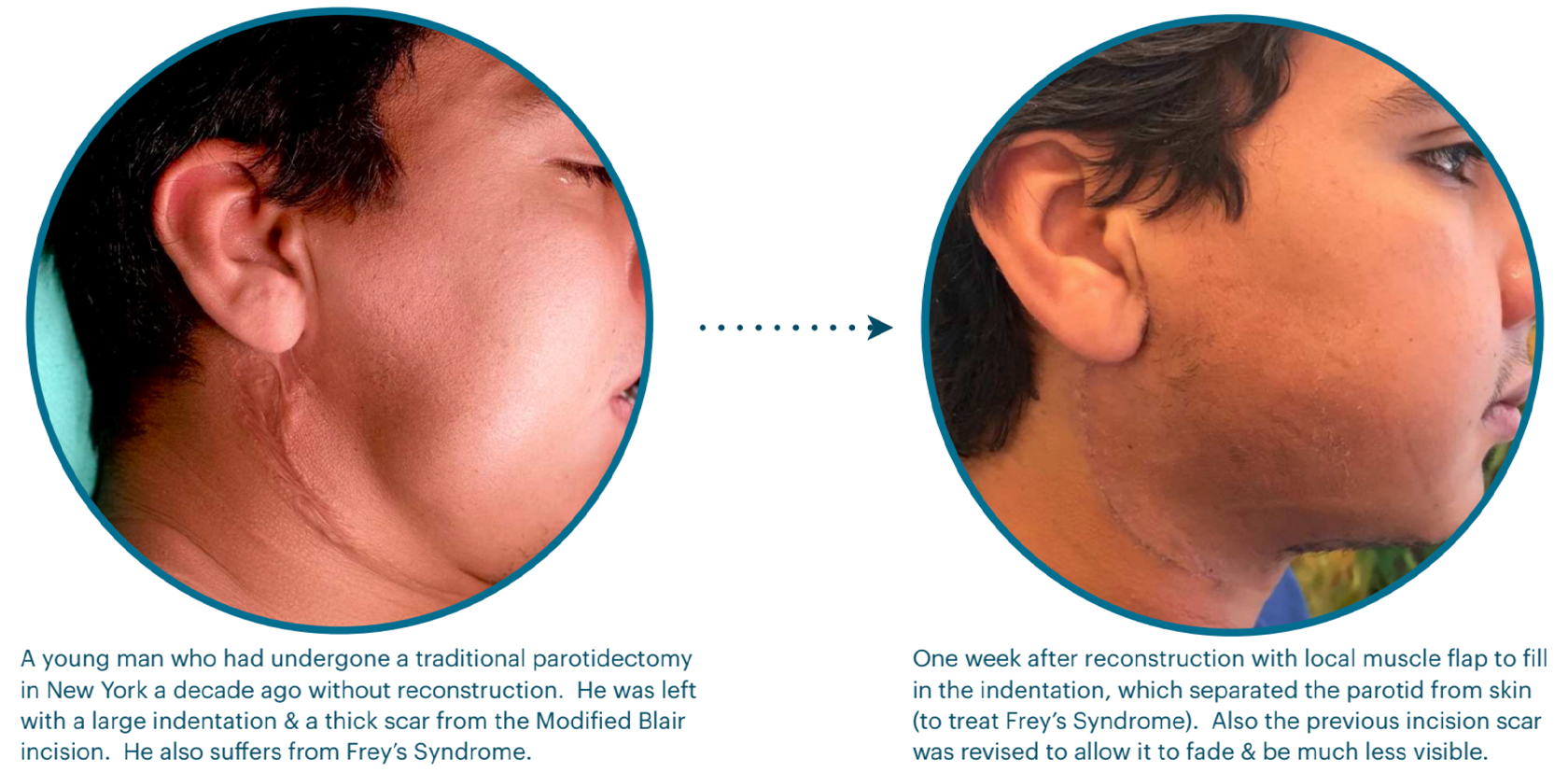
FREY’S SYNDROME
Frey’s syndrome is a permanent condition caused exclusively by parotid surgery if a reconstruction is not done. The person suffering from Frey’s will have sweating on the side of the face around the bottom half of the ear every time they eat, and even when they get hungry. Sometimes, when the
person thinks about food, it may happen. Treatments include using anti-perspirants on the face daily, every few months, injecting Botox into the parotid to stop it from producing saliva, or reconstructive surgery.
The AURICOTEMPORAL NERVE enters the parotid gland and divides into multiple branches that reach all parts of the gland. It is completely separate from the facial nerve and much smaller. The branches of the auricotemporal nerve are so small that they are not visible, even under magnification. The facial nerve does not perform any function inside the parotid gland; it only stimulates the muscles of the face. The auricotemporal nerve, on the other hand, tells the parotid gland to produce saliva and secrete it into the mouth. A tumor in the parotid gland will disrupt some of the branches and push other branches aside.
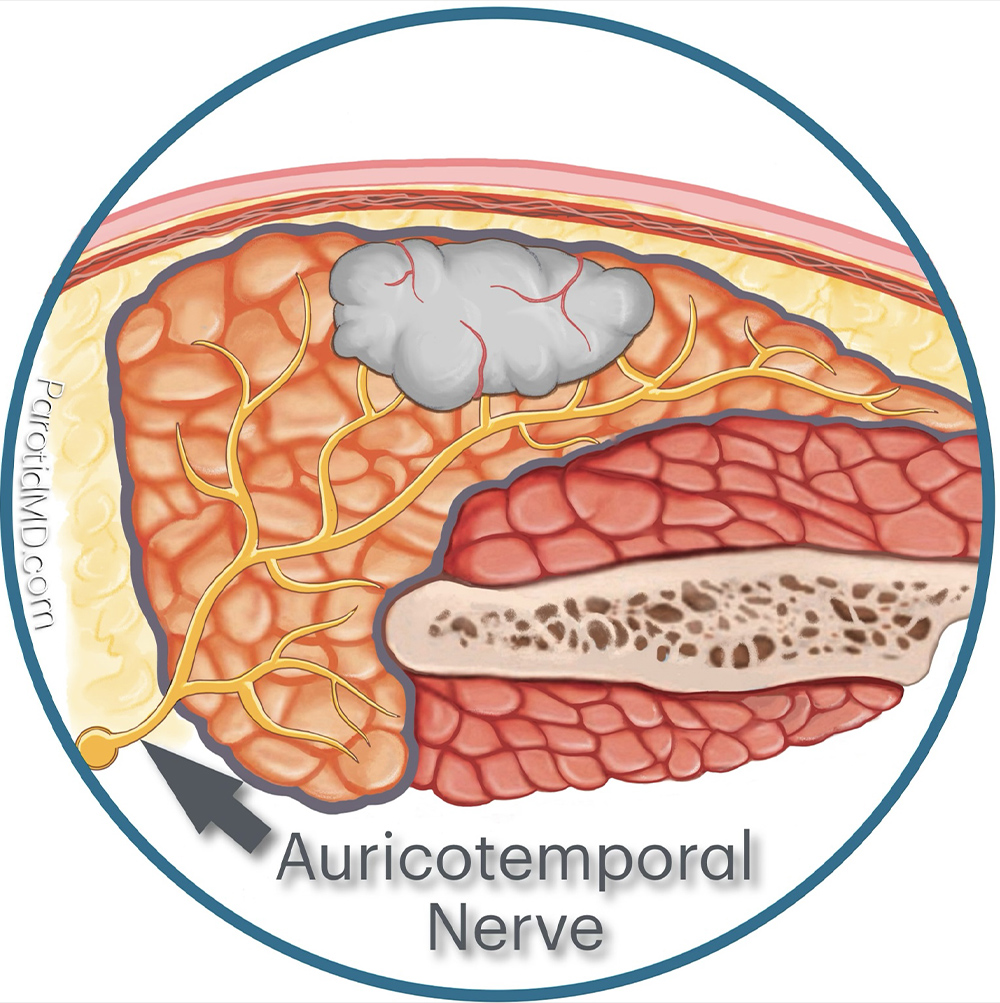
When a parotid tumor is removed many of the branches of the auricotemporal nerve are cut in the area of the surgery. Some of the cut nerve branches will scar down and not grow, and the rest will start to regenerate. The nerve fibers that sprout out of the cut edges will look for salivary tissue to attach to.
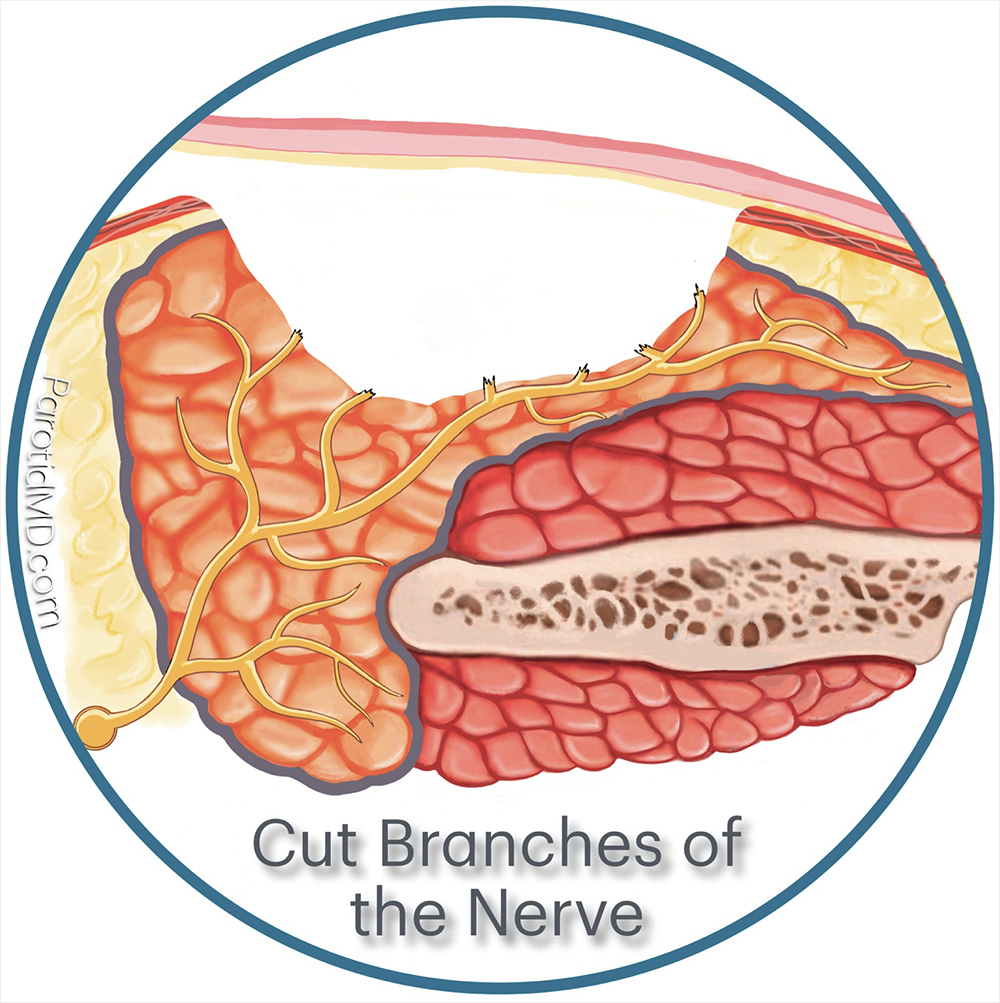
When the cut branches of the auricotemporal nerve regenerate, they grow into the skin laid down on the parotid gland. This happens when reconstructive surgery is not done to separate the parotid gland from the skin. Over time, these regenerating nerves connect to sweat glands in the skin. This occurs because sweat glands also receive nerve input from nerves similar to the auricotemporal nerve. Consequently, whenever the person is hungry or eats, the auricotemporal nerve sends a signal intended for the parotid gland to produce and release more saliva. However, the branches that have grown into the skin stimulate the sweat glands, causing the person to sweat on the side of their face.
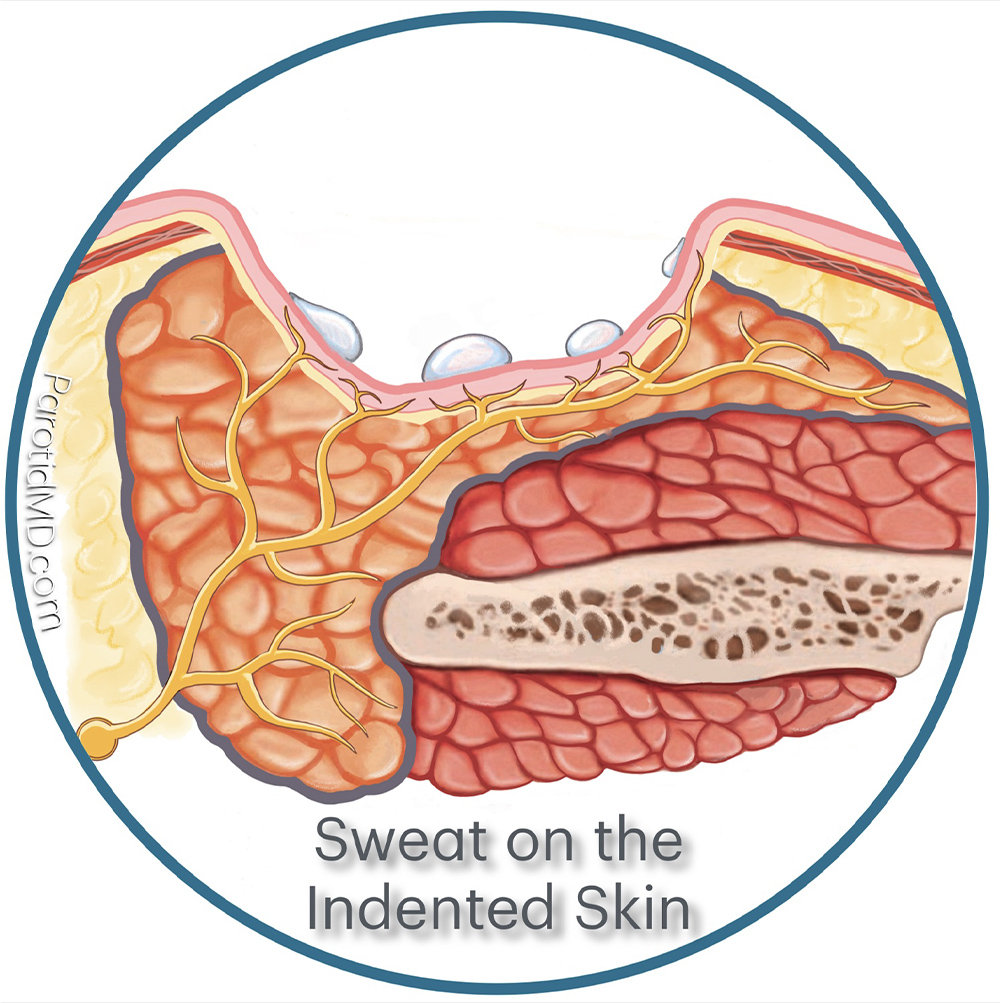
To prevent Frey’s syndrome reconstructive surgery must be done to separate the parotid gland and the cut the branches of the auricotemporal nerve from the skin. A variety of reconstructive techniques are available that can achieve this. Most work very well. In the image shown here a muscle flap was placed over the parotid gland, covering the cut branches of the auricotemporal nerve and filling the defect left by tumor removal. The SMAS layer was also preserved to give an additional layer of separation.
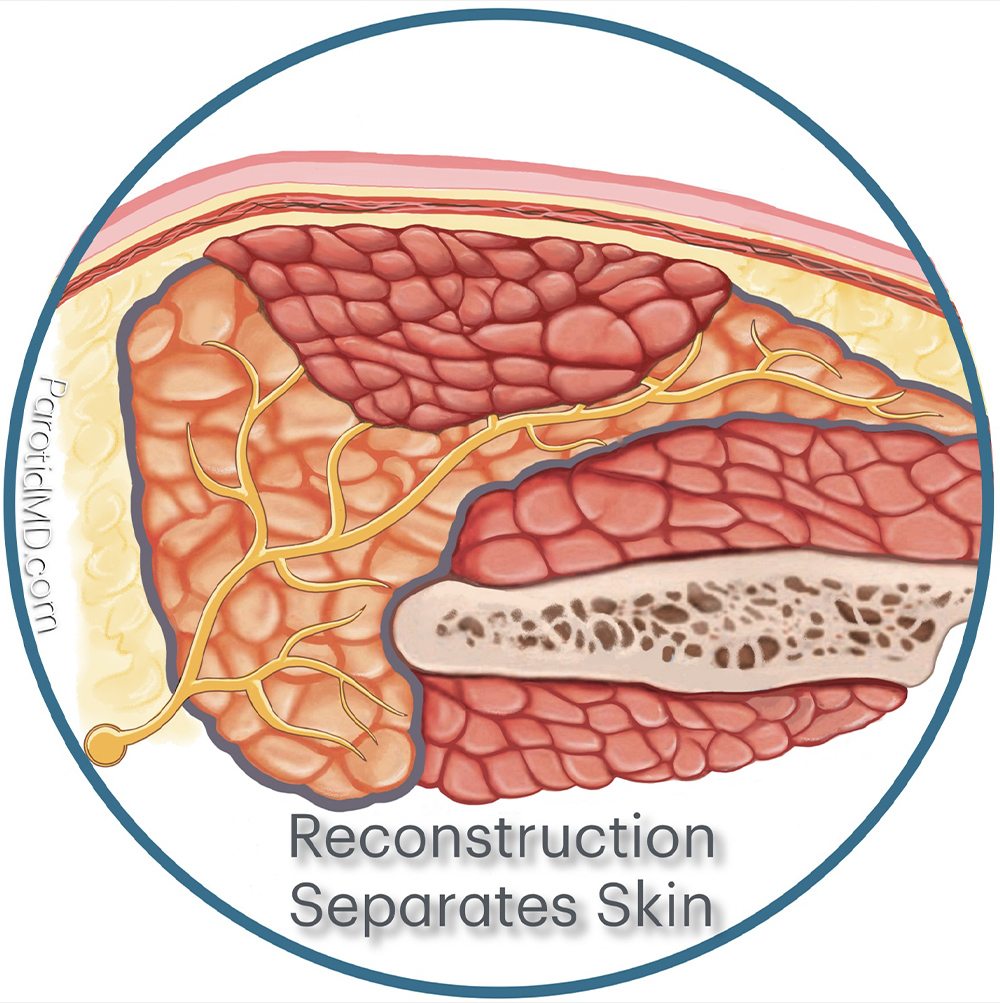
RECONSTRUCTIVE TECHNIQUES
There are a variety of different reconstructive techniques. In this section will discuss the most commonly used techniques at our CENTER. Each technique has its own particular indication based on size and location of defect. Our preference is to use local tissue to reconstruct the defect because it does not require a separate incision and we know the tissue will survive because it has blood vessels feeding it.
PRIMARY PAROTID CLOSURE & SMAS FLAP
When the tumor is small in any area of the parotid such that when it is removed with an additional amount of normal parotid tissue (to prevent tumor recurrence), the defect left behind is small then a simple reconstruction is used. By this we mean we can use the parotid gland itself for the reconstruction. In addition, in every parotid surgery if possible we reserve the SMAS fascia to use for an added layer of reconstruction.
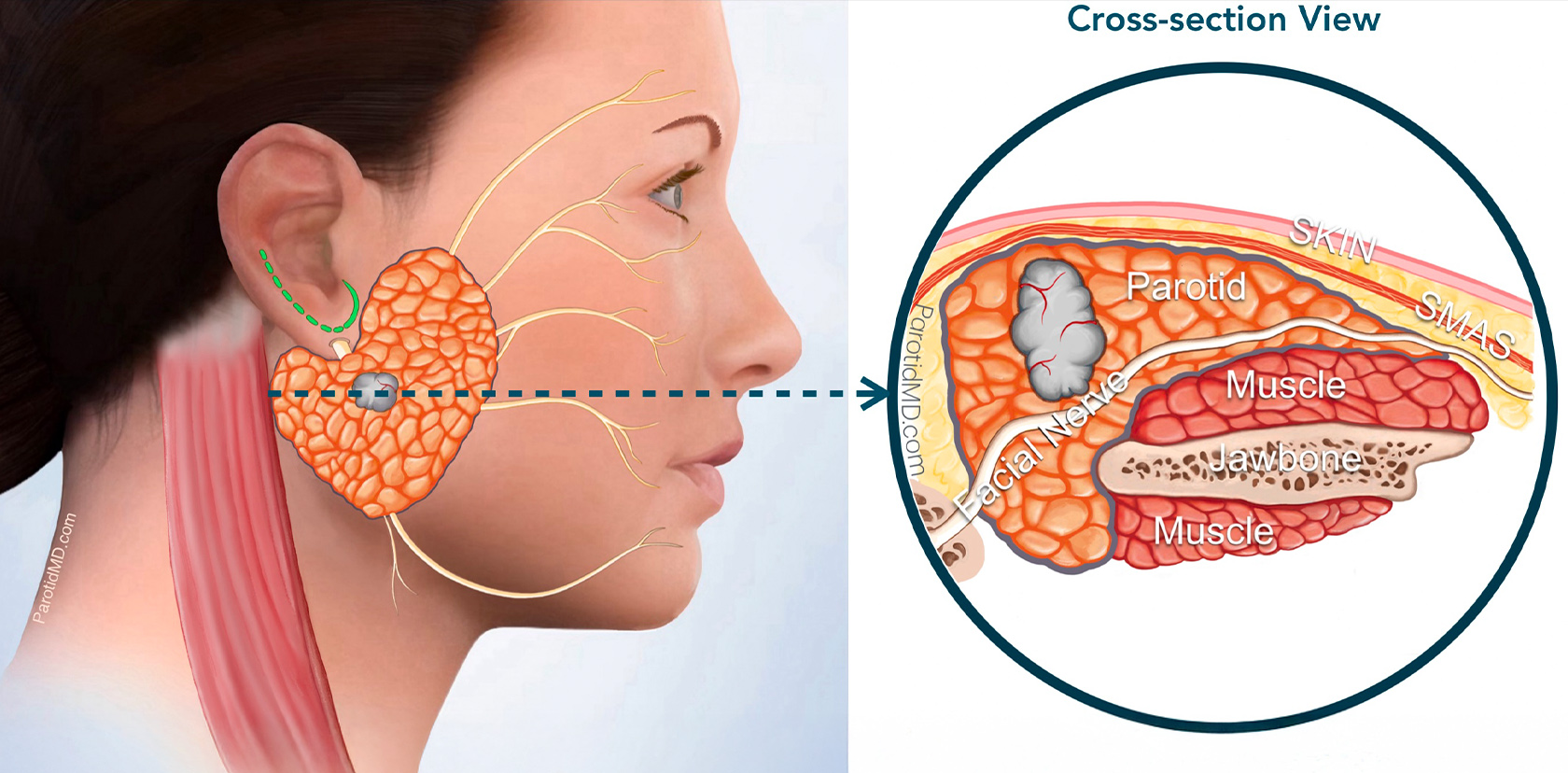
The tumor is very small. Its size has been confirmed by an imaging study (ultrasound or MRI). Cross-section view shows the size of the tumor. The first step of surgery at the CENTER is to make the incision (green line by the ear) & lift up the skin and SMAS layer.
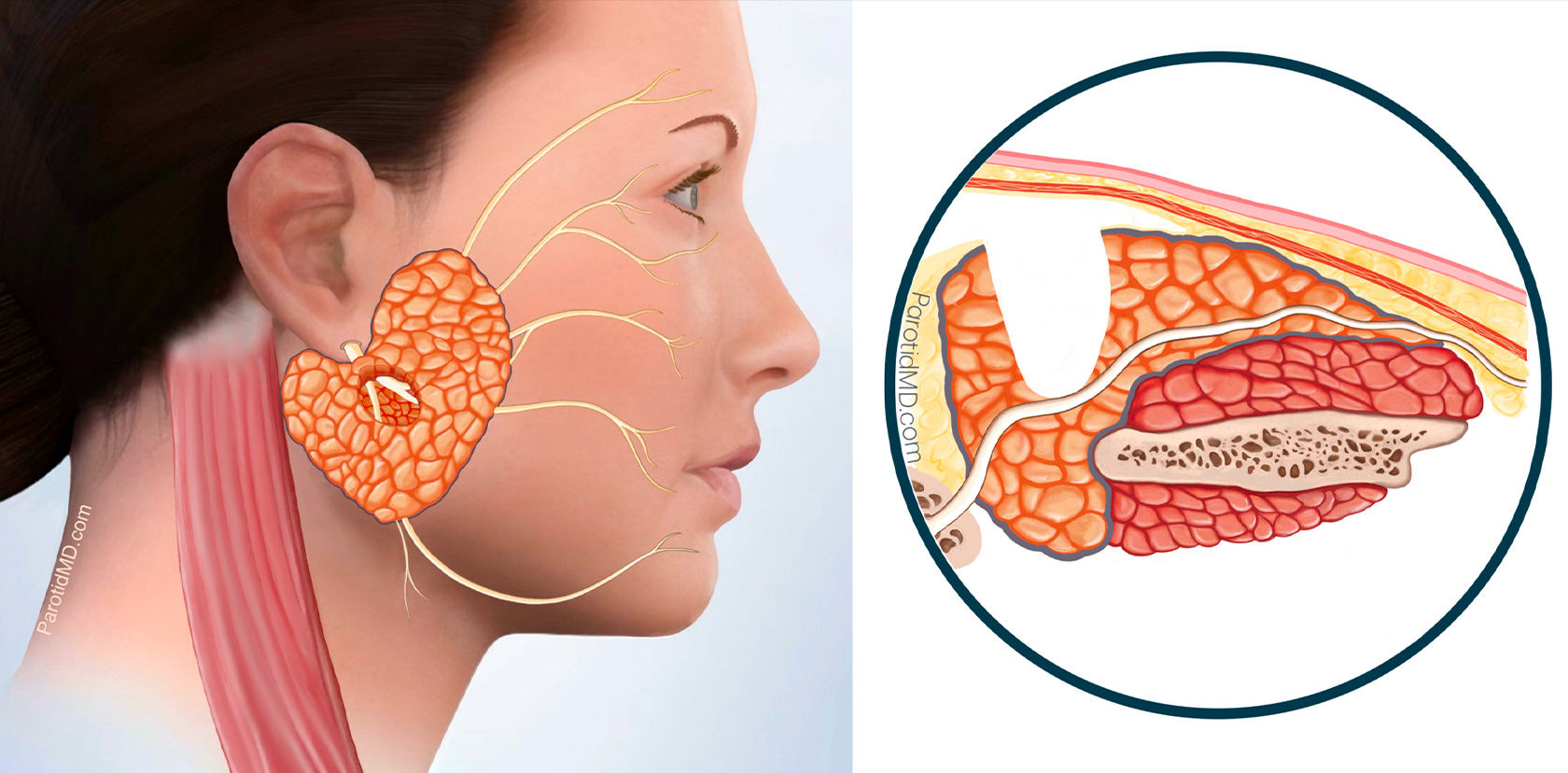
After safely & meticulously identifying the facial nerve branches the tumor and an appropriate amount of healthy parotid tissue surrounding it is removed. This is to prevent a recurrence of the tumor in the future. The defect left behind is rather small.
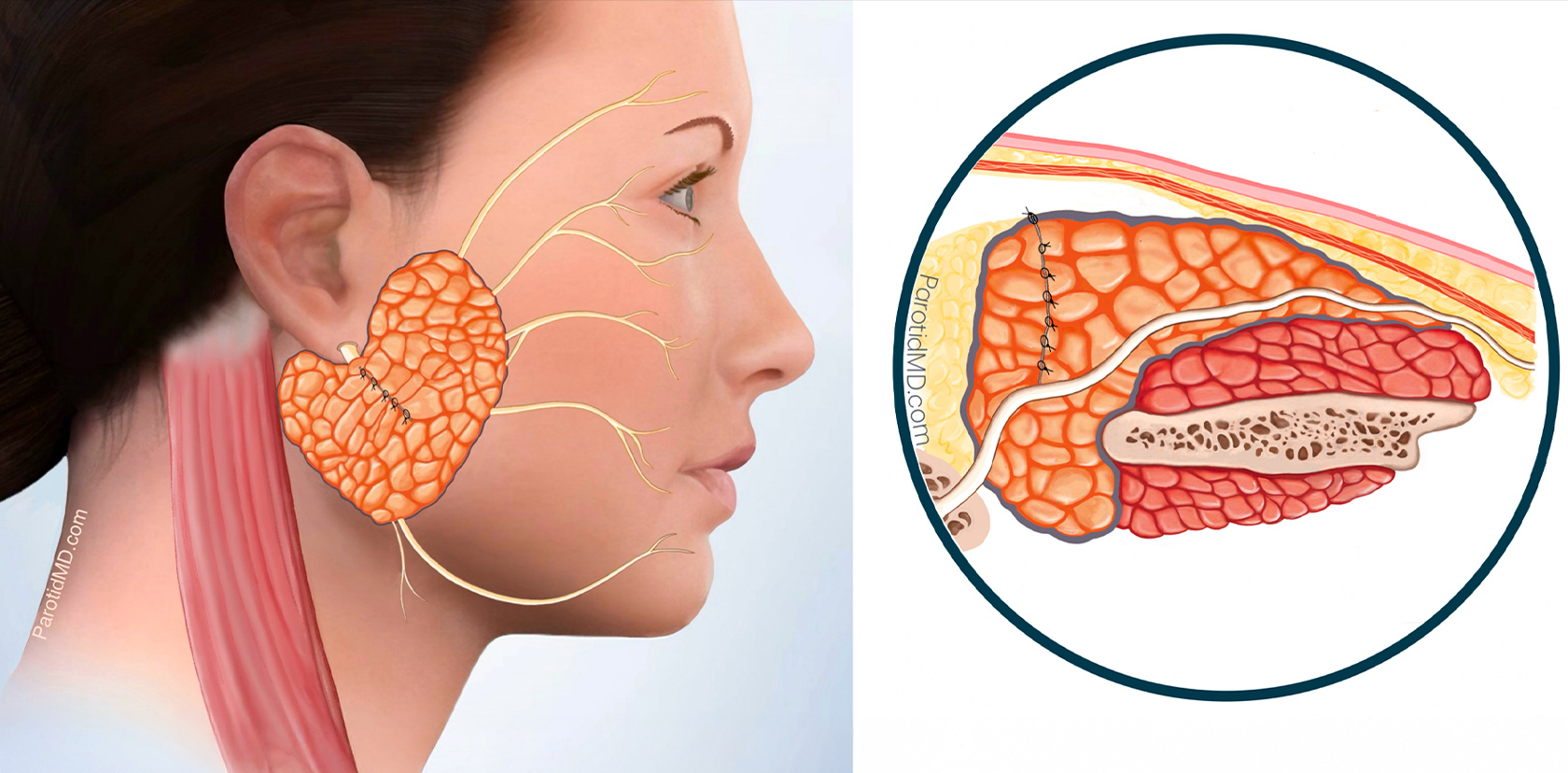
Since the defect was very small, the parotid tissue at two edges of the defect can be brought together and sutured together. This covers the facial nerve & fills in the defect. The cut auricotemporal nerve branches are facing the parotid tissue and will not have the chance to grow into the skin.
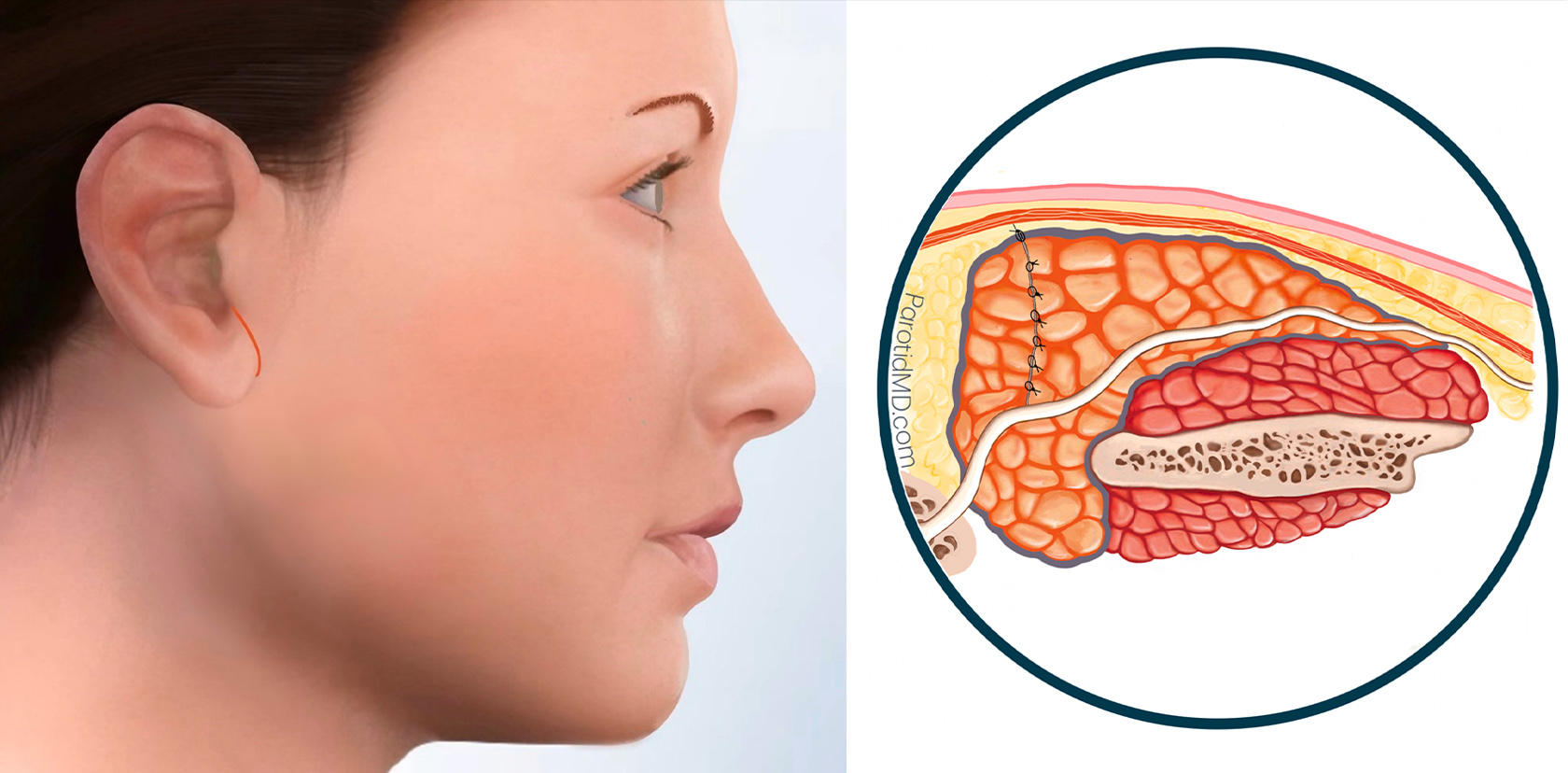
After making sure there is no blood collecting in the area of the surgery the SMAS layer is laid down over the parotid. Then the skin is placed over the SMAS layer. The SMAS layer is an added layer of separation between the parotid gland and the skin. It also creates a smooth contour on the side of the face. The skin is closed with very fine absorbable sutures under the surface.
This technique is our preferred method at the CENTER. It’s highly effective in reconstructing smaller parotid defects. It can be applied anywhere in the parotid gland, including the deep lobe. This technique causes little swelling and inflammation, resulting in significantly less discomfort. Moreover, it facilitates much faster healing. The short-term and long-term outcomes from this type of reconstruction are excellent.
SCM FLAP COMBINED WITH SMAS FLAP
When the tumor is larger than 2-3 cm, once removed, the size of the defect left behind is too large to be able to bring the two edges of the remaining parotid together and get a symmetric contour on the face. This means that we would need more substantial tissue to put into that gap. The tissue to use would need to be resilient, not dissolve away over time, and be substantial enough to fill in the defect. The STERNOCLEIDOMASTOID MUSCLE has these exact characteristics. Additionally, since we try to preserve the SMAS fascia in every parotid surgery, it can serve as an added layer for the reconstruction.
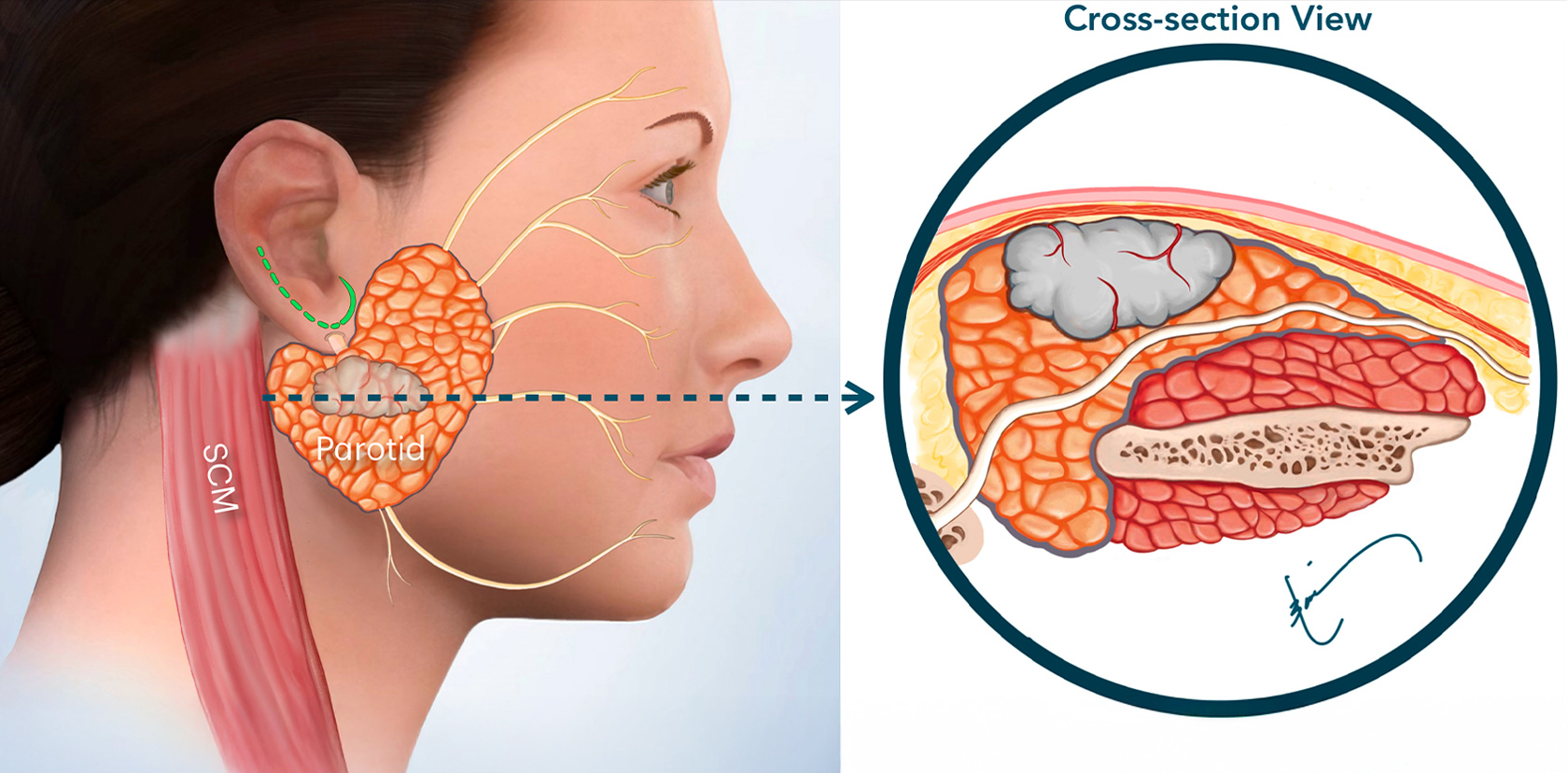
The tumor is large. Its size has been confirmed by an imaging study (ultrasound or MRI). A cross-sectional view shows the size of the tumor. The first step of surgery at the CENTER is to make the incision (green line by the ear) & lift the skin and SMAS layer.
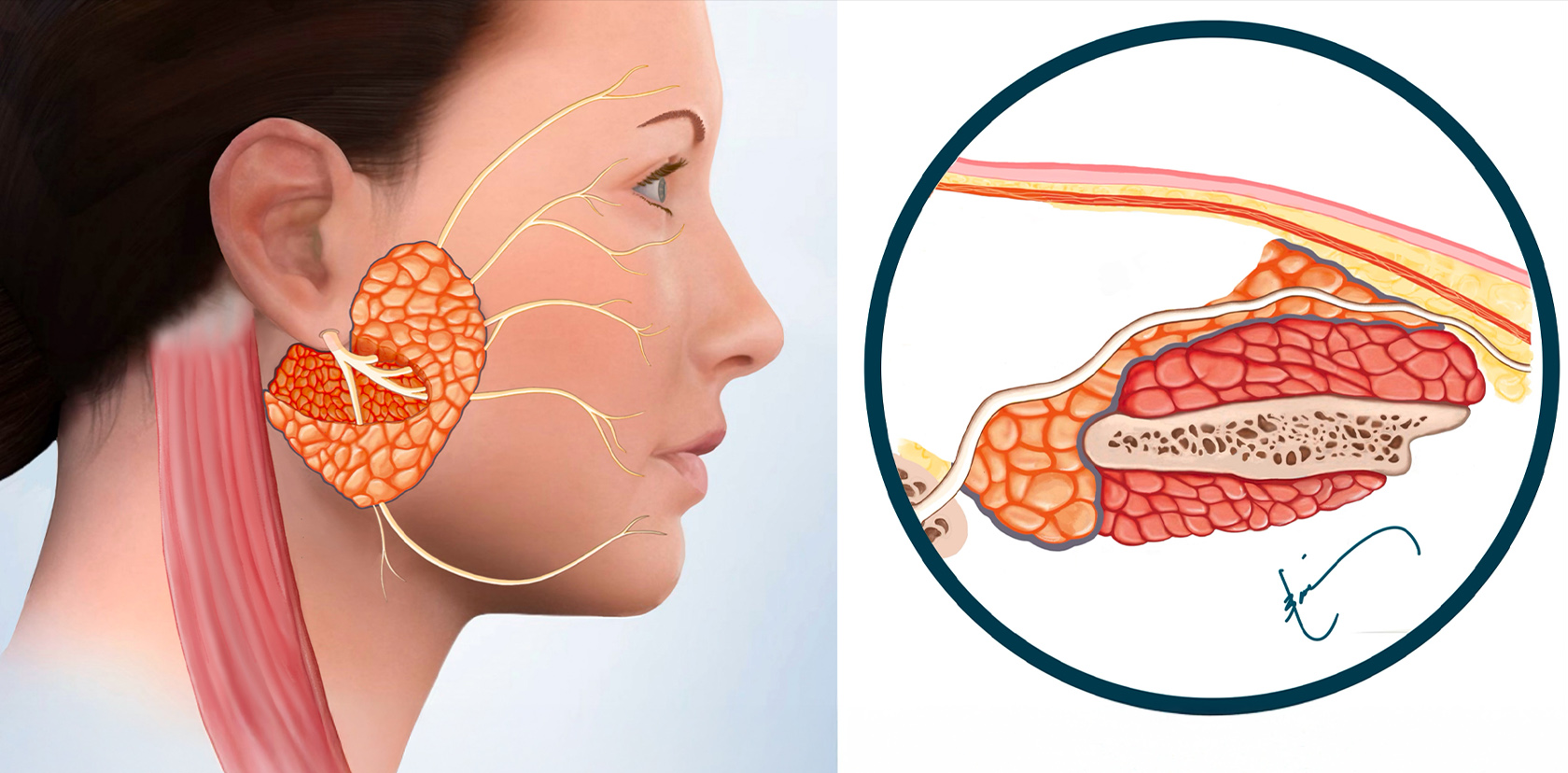
After safely & meticulously identifying the facial nerve branches, the tumor and an appropriate amount of healthy parotid tissue surrounding it are removed. This is to prevent a recurrence of the tumor in the future. The defect left behind can be rather large.
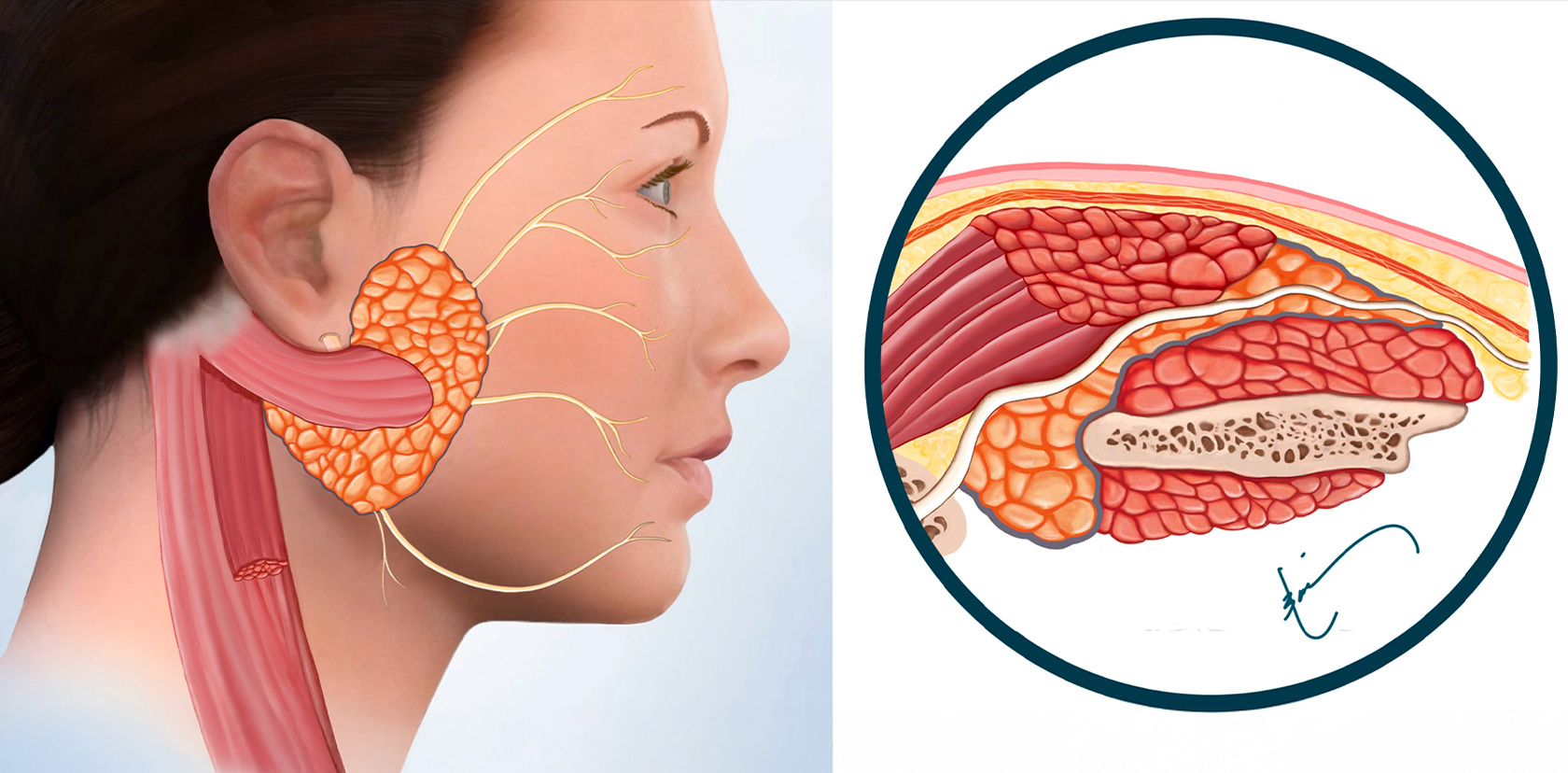
Since the defect was large, and the parotid tissue at the two edges of the defect cannot be brought together, a portion of the sternocleidomastoid muscle (SCM) is used for reconstruction. The SCM flap is attached at one end to the rest of the muscle, where it gets blood flow from, & the other end is used to cover the facial nerve & fills in the defect. This separates the parotid from the skin.
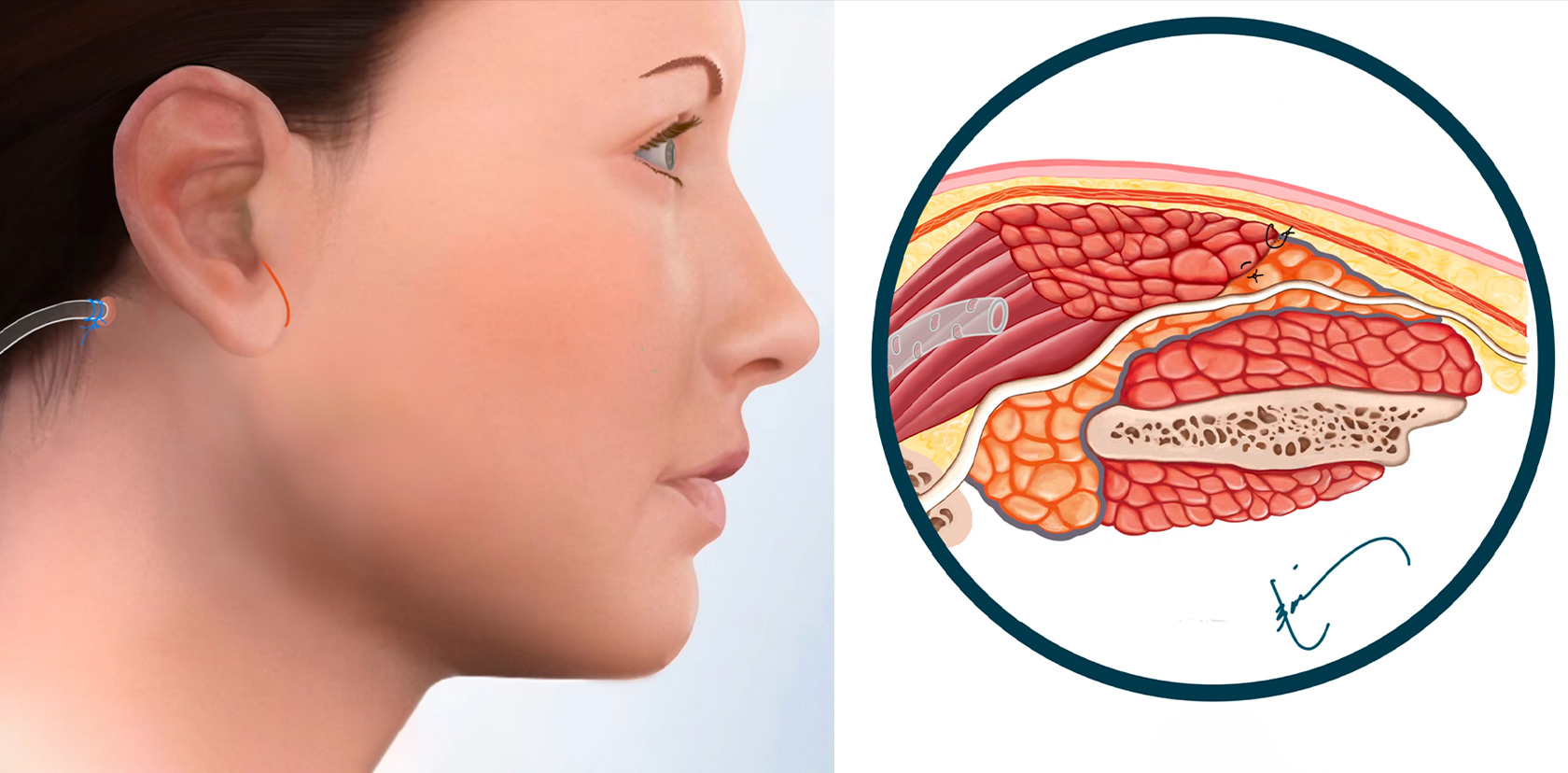
The SMAS layer is laid down over the SCM flap that is on the parotid, filling in the defect. Then the skin is placed over the SMAS layer. The SMAS layer is an added layer of separation between the reconstructed parotid gland and the skin. It also creates a smooth contour on the side of the face. A drain is used in larger defects when the SCM flap is utilized because there is more fluid that accumulates under the surface & the drain removes it. The skin is closed with very fine absorbable sutures under the surface.
This technique is our preferred approach at the CENTER when the tumors are larger, resulting in a significant defect and indentation. It is highly effective in reconstructing larger parotid defects, even with tumors significantly larger than those depicted in the images above. Since the SCM is adjacent to the parotid gland, access to the muscle is relatively straightforward and can be achieved easily through the micro-parotidectomy approach. Since only a small portion of the muscle is required for this reconstruction, the SCM flap does not cause any weakness or limitation of neck movement. The drain remains in place for approximately 2 days and can be managed effectively at home without the need for hospitalization. The healing process is relatively quick. This type of reconstruction creates a very symmetrical shape on the side of the face and, over time, becomes soft, resembling normal facial tissue. The short-term and long-term outcomes from this approach are excellent.
FAT GRAFT COMBINED WITH SMAS FLAP
Fat grafts have two primary indications in parotid reconstruction:
1) When the defect is located in the front or upper part of the parotid gland and is too large for the two edges to be sutured and closed together. This area is too far away from the sternocleidomastoid muscle (SCM), and an SCM flap would either have to be overlaid on normal parotid tissue, which would appear bulky, or it would necessitate removing additional parotid tissue in the back to allow the SCM flap to be brought in.
2) When the individual’s face is large, and the SCM flap alone is insufficient to fill in the defect adequately. In such cases, all three components—the SCM muscle, fat graft, and SMAS flap—are used to create symmetry and harmony.
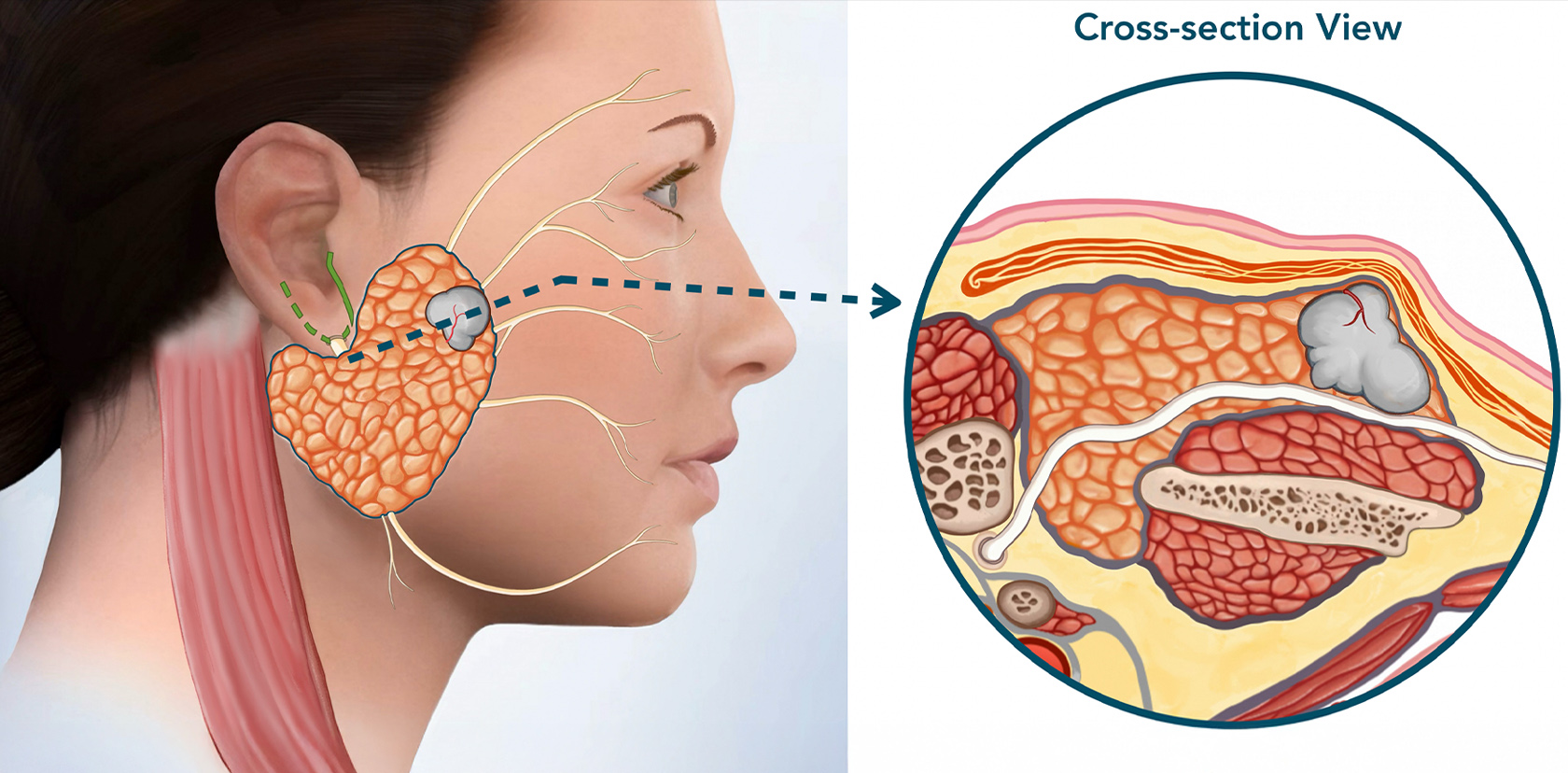
The tumor is small. It can be easily felt & is seen bulging the skin of the cheek. Its size has been confirmed by an imaging study (ultrasound or MRI). A cross-sectional view shows the size of the tumor. The first step of surgery at the CENTER is to make the incision (green line by the ear) & lift up the skin and SMAS layer.
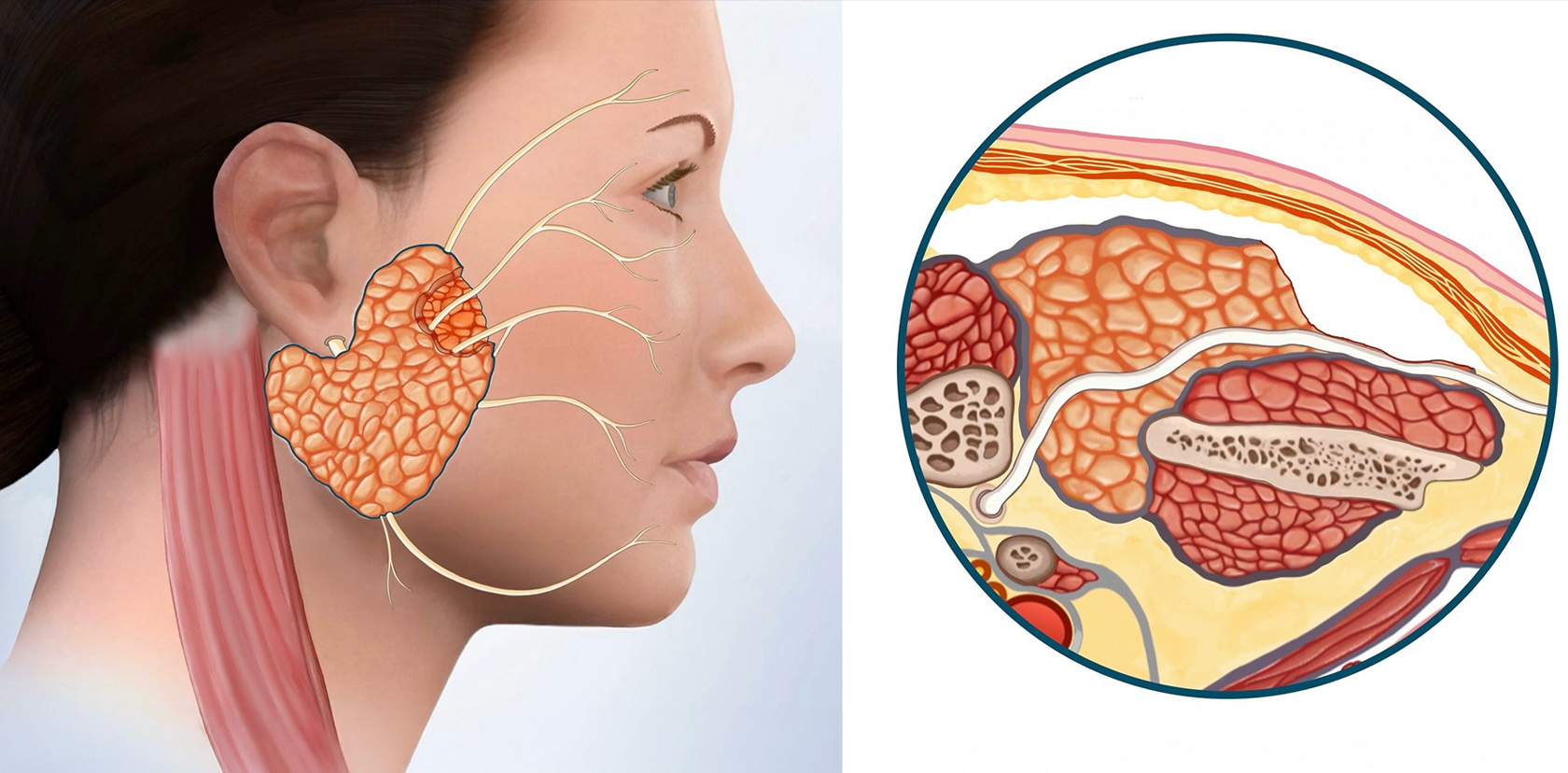
The fat graft is placed in the defect. Usually 30% more than needed because fat shrinks in time. The SMAS layer is laid down over the fat graft & parotid, creating a smooth contour. Then the skin is placed over the SMAS layer. The SMAS layer is an added layer of separation between the reconstructed parotid gland and the skin. The skin is closed with very fine absorbable sutures under the surface.
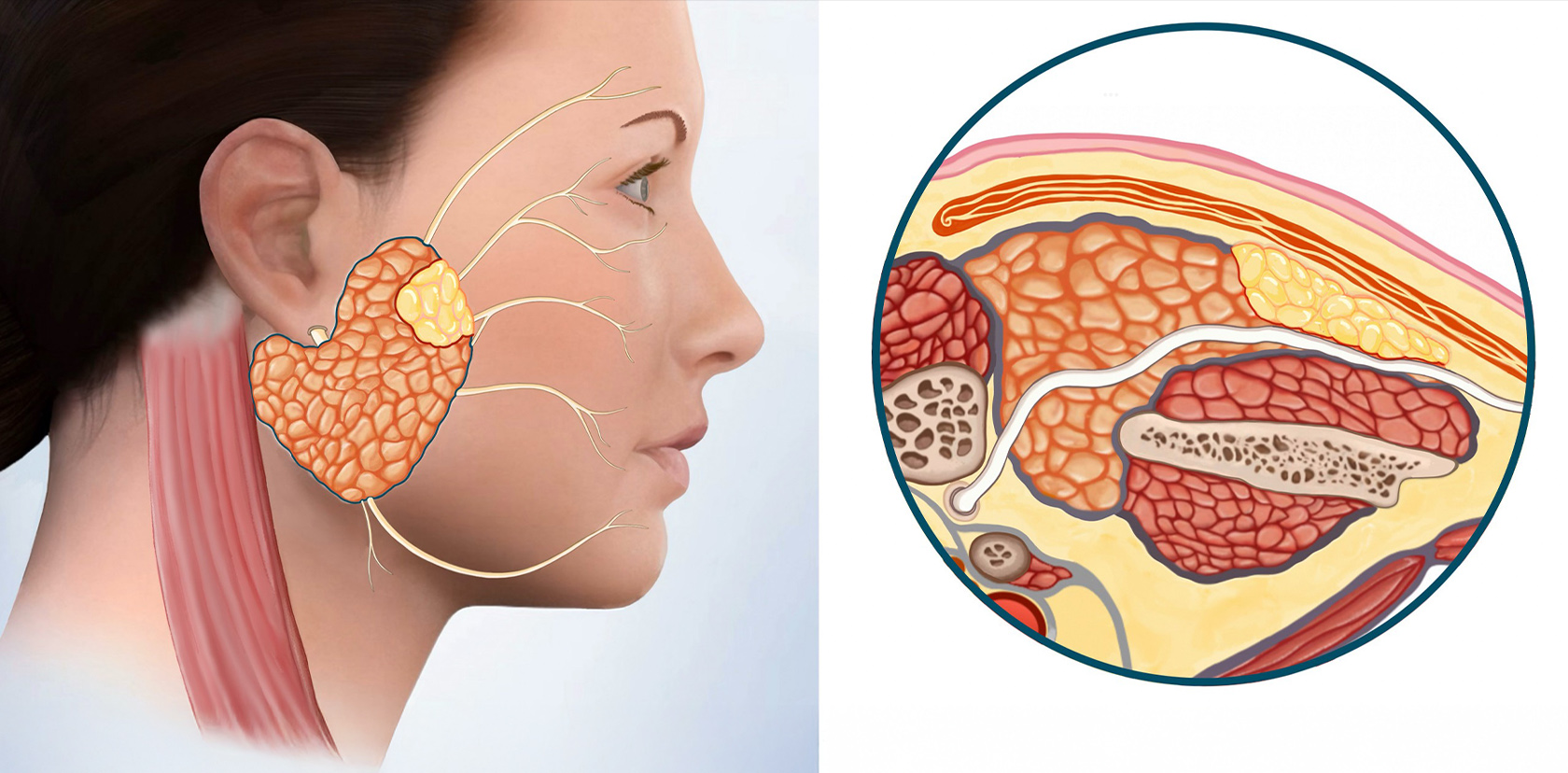
Since the defect was large, and the parotid tissue at the two edges of the defect cannot be brought together, a portion of the sternocleidomastoid muscle (SCM) is used for reconstruction. The SCM flap is attached at one end to the rest of the muscle, where it gets blood flow from, & the other end is used to cover the facial nerve & fills in the defect. This separates the parotid from the skin.
Fat grafts are highly effective in reconstructions. They are relatively straightforward because fat is malleable and easy to shape into the defect. However, the fat must be harvested from the abdomen, necessitating a small incision in the belly button. Consequently, the grafted fat will inevitably undergo partial absorption and shrinkage over time before it can grow blood vessels into it to bring it nutrition. To account for these factors, the amount of fat used is typically 30% higher than the size of the defect. This makes fat grafting a little less reliable because the surgeon has to account for changes over time that are not always the same in all people.
GALLERY RECONSTRUCTION
PRIMARY PAROTID CLOSURE & SMAS FLAP
Before
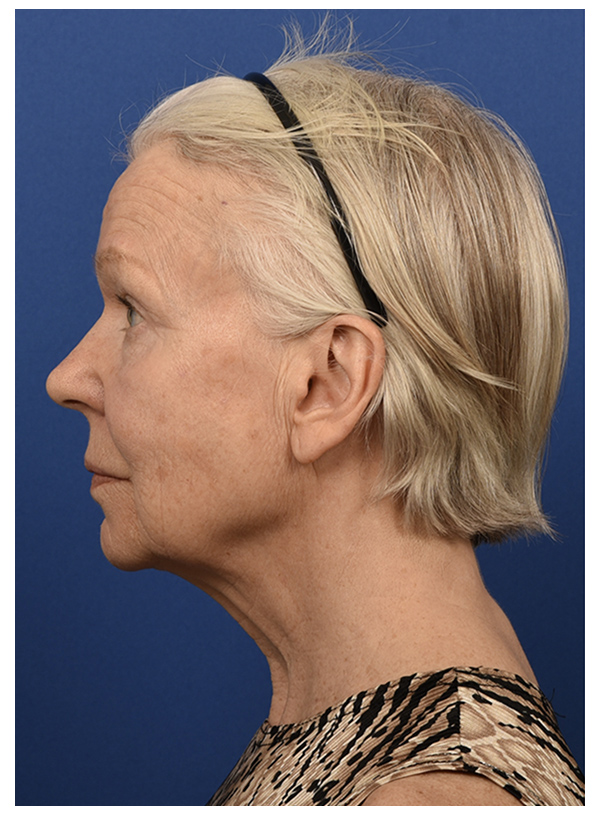
After - 3 Weeks
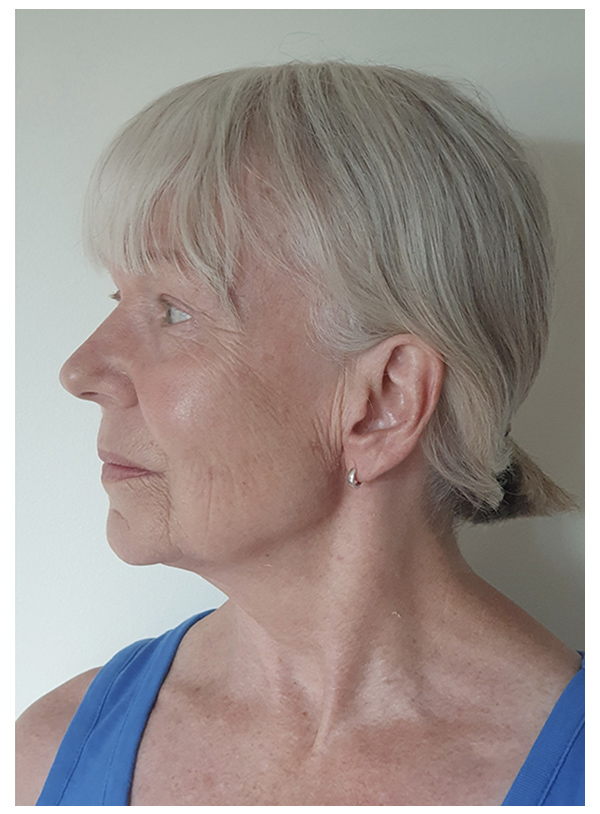
MUSCLE FLAP & SMAS FLAP
Before
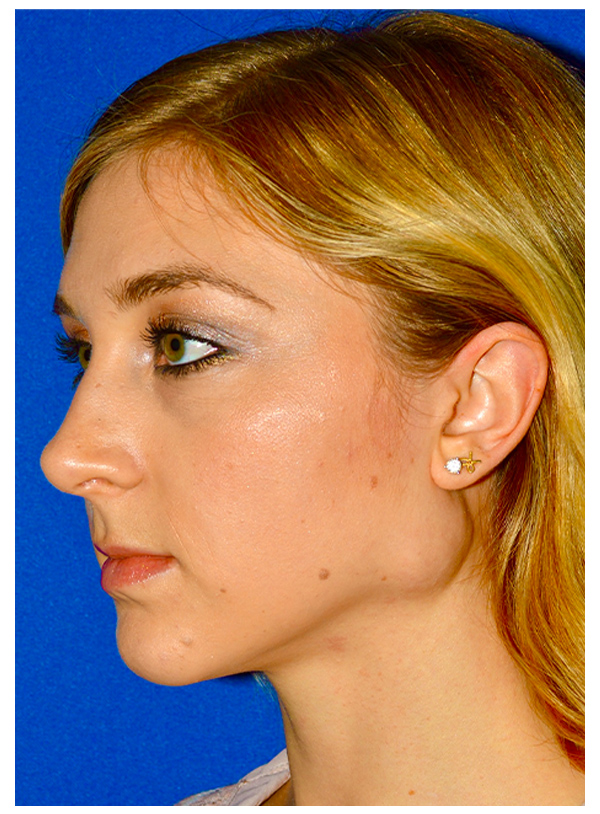
After - 7 days
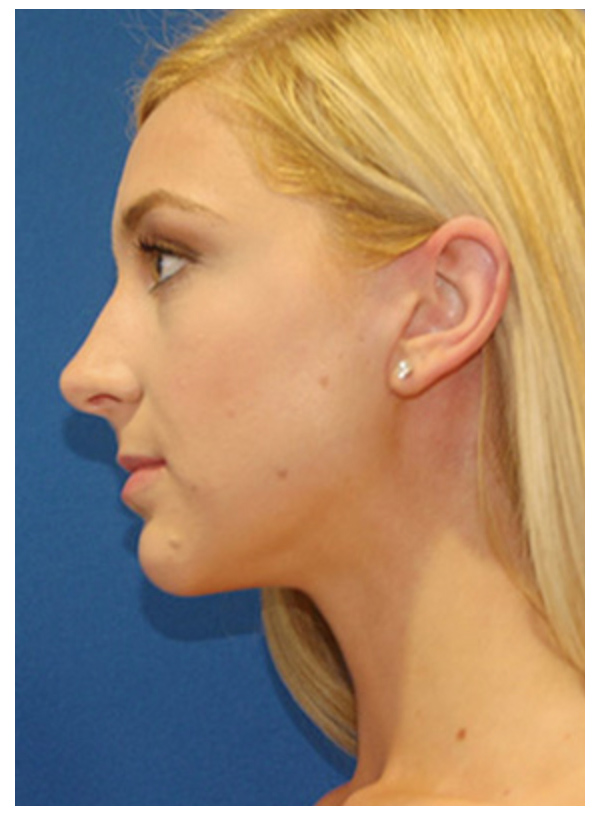
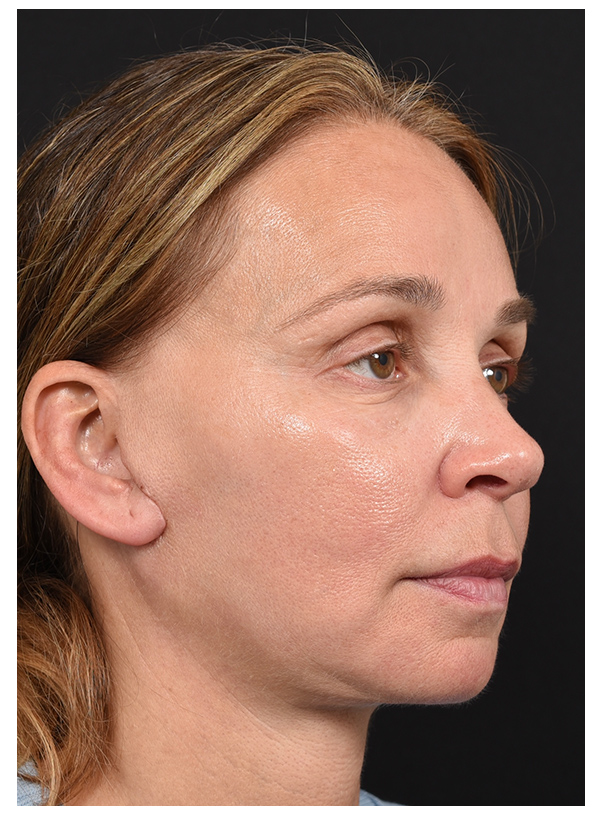
FAT GRAFT COMBINED WITH SMAS FLAP
Before
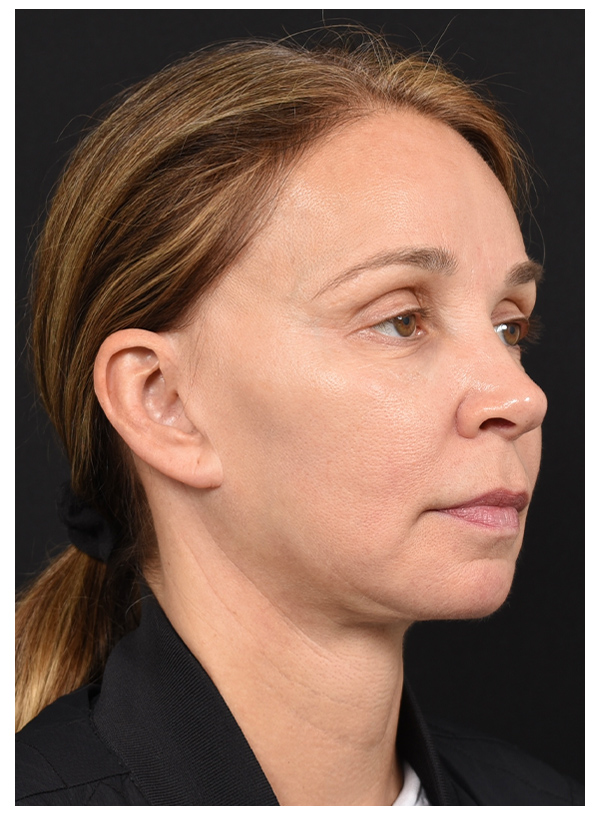
After - 4 Days
MUSCLE FLAP & SMAS FLAP
Before
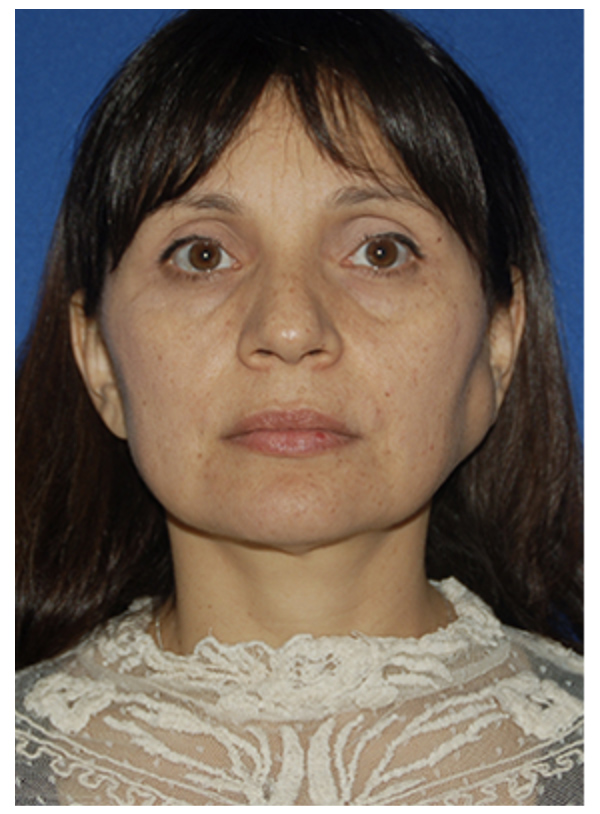
After- 1 Month

PRIMARY PAROTID CLOSURE & SMAS FLAP
Before
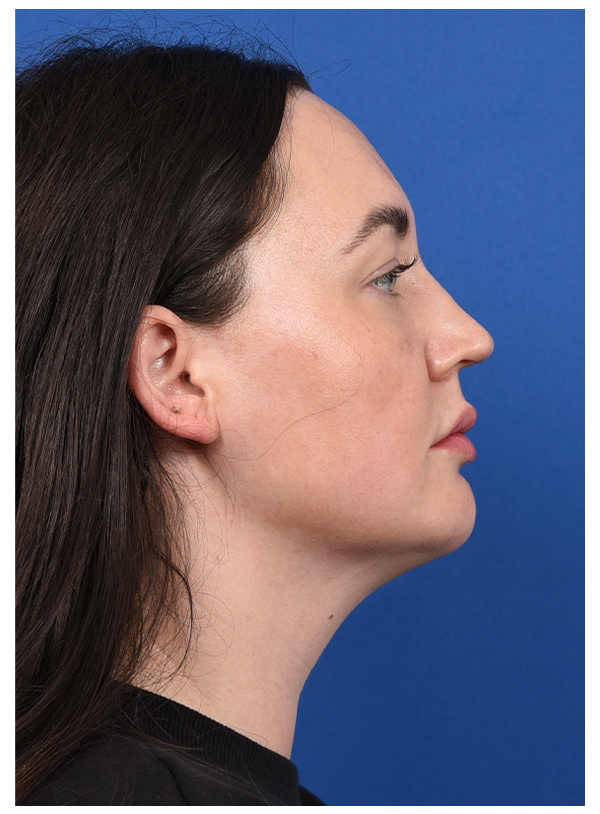
After - 1 Month
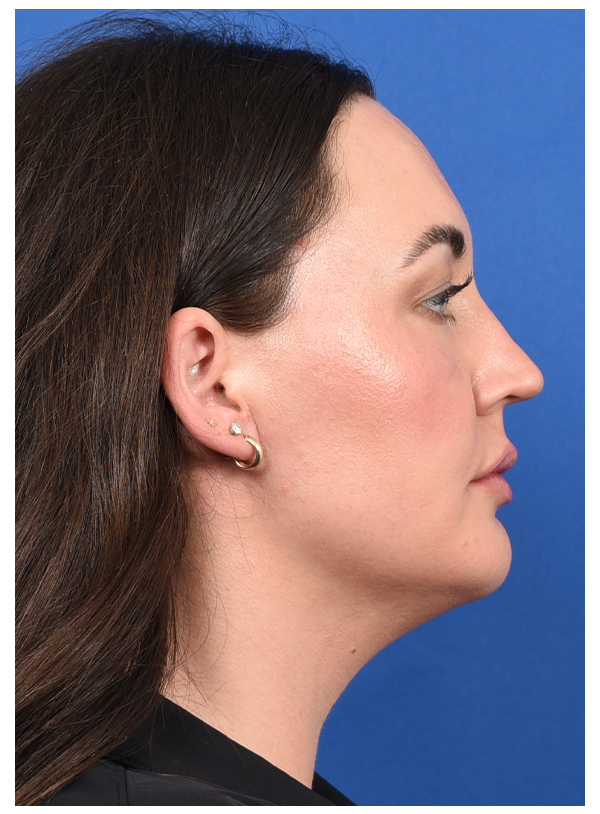
MUSCLE FLAP & SMAS FLAP
Before
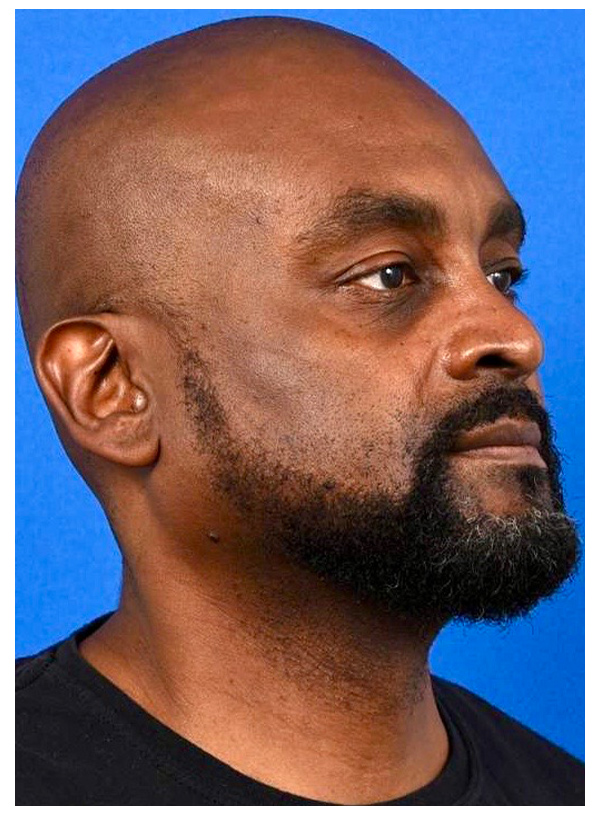
After - 2 Weeks

FAT GRAFT COMBINED WITH SMAS FLAP
Before

After - 4 Days
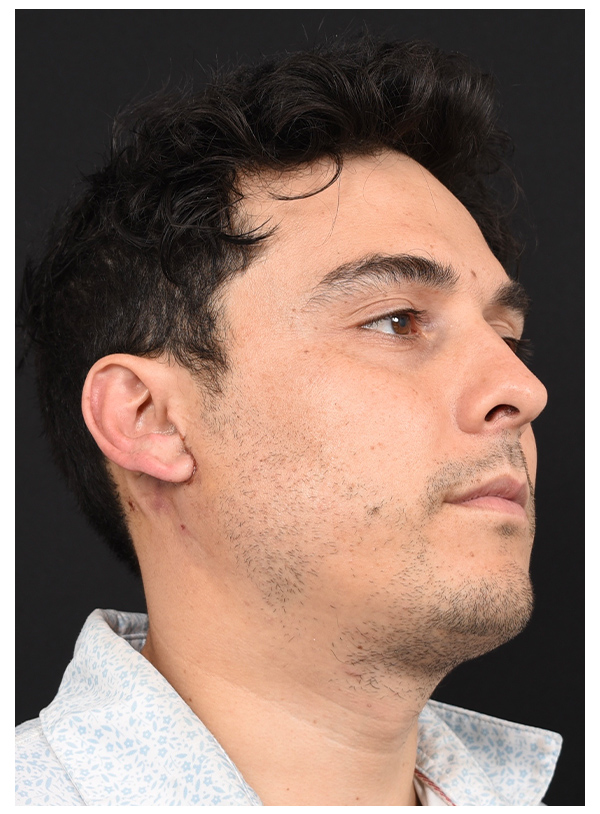
MUSCLE FLAP & SMAS FLAP
Before

After- 2 Weeks

PRIMARY PAROTID CLOSURE & SMAS FLAP
Before

After - 3 days
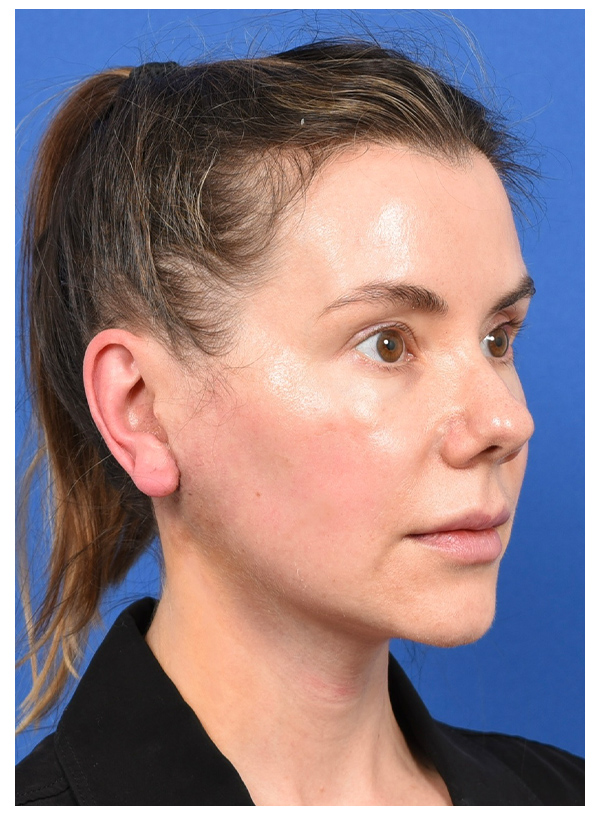
MUSCLE FLAP & SMAS FLAP
Before

After - 1 Weeks

MUSCLE FLAP & SMAS FLAP
Before
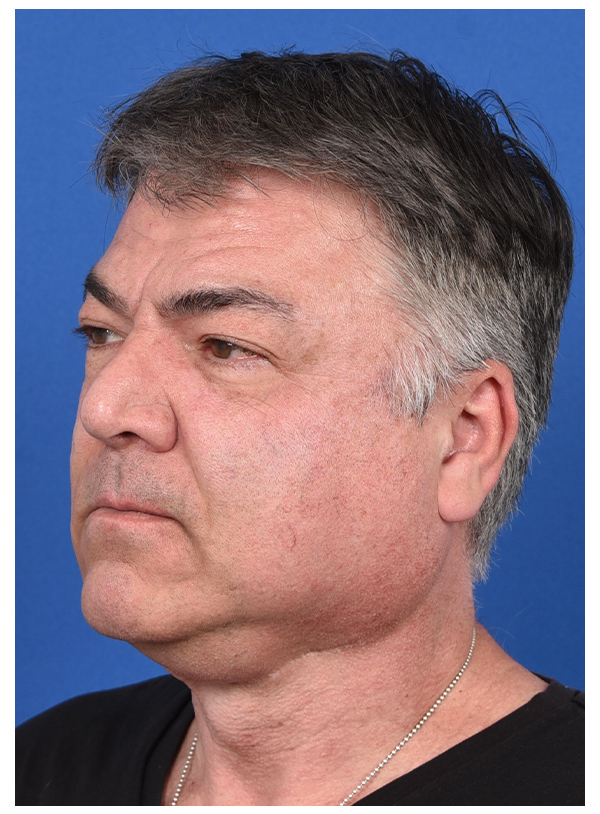
After- 1 Month

PRIMARY PAROTID CLOSURE & SMAS FLAP
Before - with marking of tumor & incision
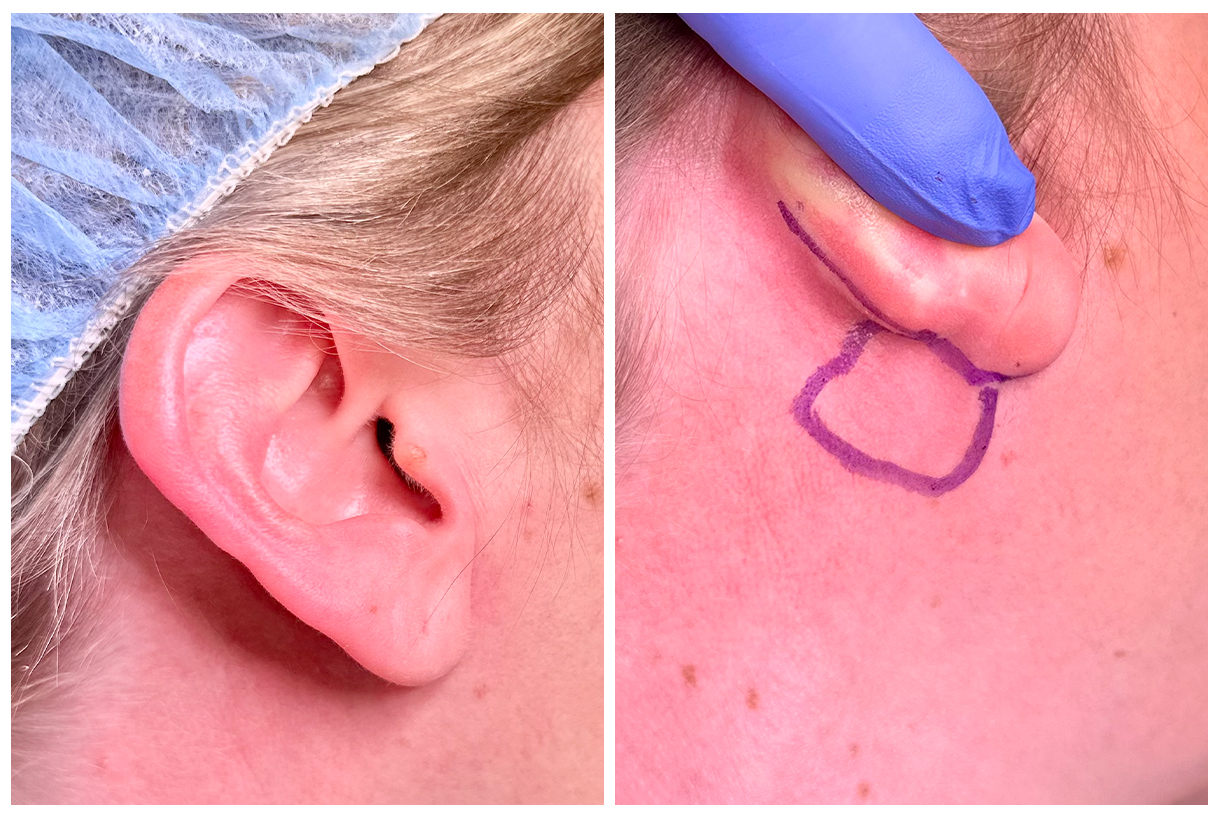
After - 1 Week. (Pictures taken at home)
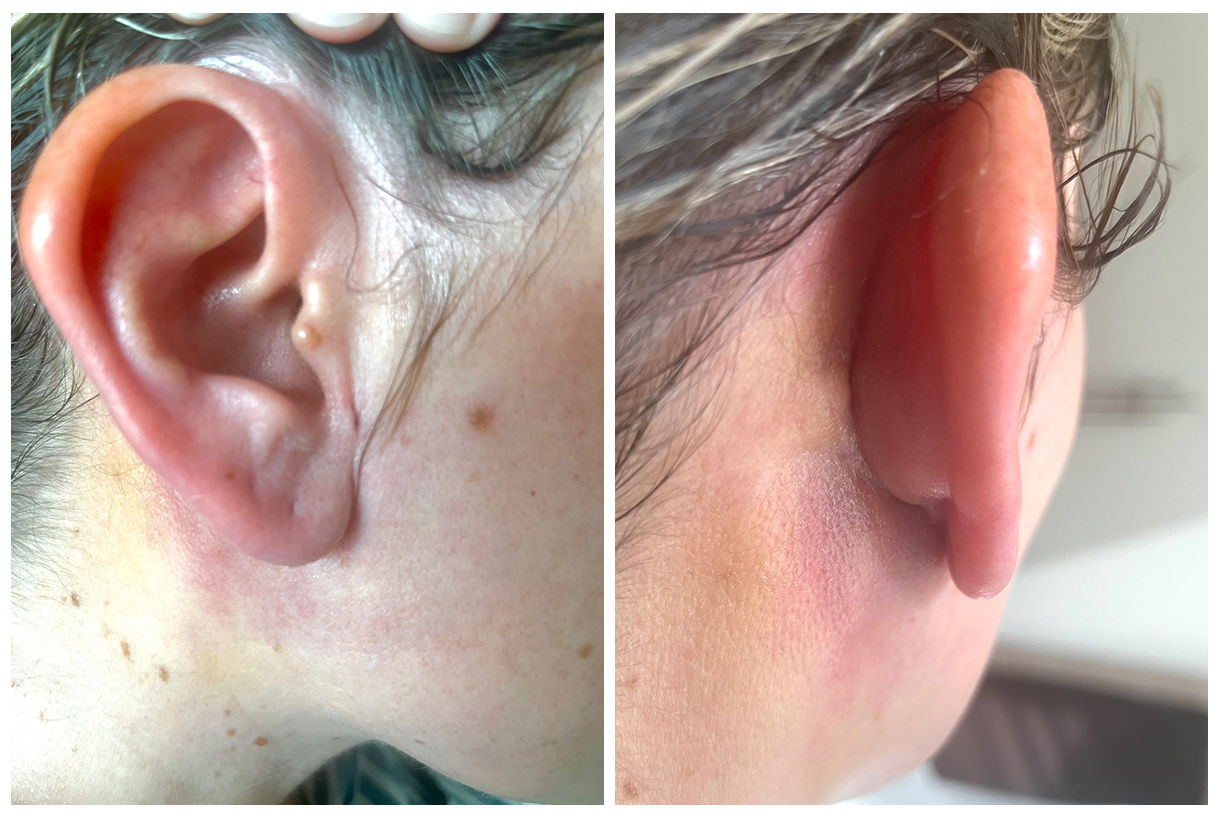
After - 1 Week (2024)
FREQUENTLY ASKED QUESTIONS
Do all parotidectomies require reconstruction?
Yes, they all do, but to different degrees. The smaller the tumor, the more minimal the reconstruction. But the reconstruction is necessary to prevent deformity and Frey’s syndrome. Both of which will develop months later.
Is the reconstruction always done by a plastic surgeon?
Not always. At the CENTER, when the smaller benign tumors or cancers are removed, and therefore the defect is small, then the reconstruction is done by Dr. Larian alone. In the cases when the tumors are very large, Dr. Azizzadeh (the plastic surgeon) will also be involved to perform more complex reconstructive surgery.
Is the SMAS layer always used for the reconstruction?
When the SMAS layer is available, it is used for reconstruction. However, sometimes the tumor involves the SMAS layer and, as such, is removed along with the tumor.
Is the reconstruction always done by a plastic surgeon?
Not always. At the CENTER, when the smaller benign tumors or cancers are removed, and therefore the defect is small, then the reconstruction is done by Dr. Larian alone. In the cases when the tumors are very large, Dr. Azizzadeh (the plastic surgeon) will also be involved to perform more complex reconstructive surgery.
Is a drain always used for parotid reconstruction?
No. When the reconstruction includes a muscle flap, then a drain is used because the edges of the muscle flap ooze some fluid that needs to be removed. Otherwise, the fluid would collect under the skin and would bulge out of the skin, which would delay healing and possibly get infected.
How much of the SCM muscle is used for a muscle flap?
Obviously, the answer depends on how big the area to be reconstructed is, but generally speaking, no more then 15% of the muscle is necessary to reconstruct the parotid defect. With 85% of the muscle being in place, it does not lose strength or range of motion. Although immediately after surgery, the person would feel tightness, the tightness improves after several weeks. At 3 weeks after surgery, our patients are encouraged to do neck stretches.
Is the SCM the only muscle used for flaps in the parotid?
In simple parotidectomies, meaning those that don’t involve removing any of the jawbone or skull bone (reserved for advanced cancers), then the SCM is the ideal muscle flap. This is because SCM is large and has blood vessels feeding it from above and below, which makes it hardy and versatile. The consistency of this muscle flap is also very similar to the tissue in the area of the parotid, so once healed, touching the area will feel close to normal.
Will the person know in advance that they will need a muscle flap?
Yes, in most cases when the tumor is large, and the parotid cannot be primarily put together, then our team will be able to predict in advance that they will use the SCM flap. But in some cases, where the size of the tumor is not very large (borderline), then there’s a chance that a simple closure will work; Dr. Larian will have to figure that out during surgery.

Meet The Team
Led by board-certified parotid surgeon, Dr. Babak Larian, our team of specialists has decades of experience successfully diagnosing and treating diseases of the parotid glands with minimally invasive procedures. Distinguished by our compassionate care and cutting-edge techniques, the CENTER has developed a reputation for delivering the best parotid tumor surgery available.